About Us
The Mom & Mitchell Foundation is a non-profit organization dedicated to fostering mental wellness and improving outcomes in treatment of mental health disorders and disease.
- Raising awareness and educating the public about mental health issues.
- Changing the stigma surrounding mental health disorders and disease.
- Encouraging a compassionate approach to those facing mental health challenges.
- Developing & promoting activities that enhance mental health and wellness.
- Supporting public policies and initiatives that seek to improve mental health and wellness.
- Reducing the morbidity and mortality resulting from psychological and psychiatric disorders and disease, including suicide and drug overdose.
Board of Directors

Timothy Jones, MD founded The Mom & Mitchell Foundation in 2021. He knows personally about the profound and devastating effects of mental health disorders on family, friends, and communities. In Tim’s family alone, he has lost his maternal grand mother, his mother, and his son, Mitchell, to suicide.
In his 30 years of medical practice as a plastic surgeon and ear, nose, and throat physician, Dr. Jones has experienced first hand the impact of both mental health and physical health, and how they are intertwined in keeping people well.
Death from suicide and drug overdoses are rising.The well intentioned treatments for Covid-19 pandemic have led to more mental health disorders as a result of social isolation, job loss, financial insecurity, and loss of friends and family to the virus. Mental health and wellness needs to be a top health priority. Tim started The Mom & Mitchell Foundation to help change the outcomes in the treatments of mental health disorders and diseases.

Marcus Engel, M.S., CPXP, CSP is a Certified Speaking Professional & author whose messages provide insight and strategies for excellent patient care. His keynote presentation, “The Other End of the Stethoscope” has been witnessed by tens of thousands of healthcare professionals and his books are used in scores of nursing and allied health programs to teach the basic foundations of caregiving.
As a college freshman, Marcus Engel was blinded and nearly killed after being struck by a drunk driver. Through two years of rehab, over 350 hours of reconstructive facial surgery and adaptation through a multitude of life changes, Marcus witnessed the good, the bad and the profound in patient care.
Marcus has authored four books and is currently at work on a fifth. He holds a B.S. in sociology from Missouri State University and a M.S. in Narrative Medicine from Columbia University in the city of New York.
In 2017, Marcus was awarded an honorary doctorate from the Philadelphia College of Osteopathic Medicine and is currently an adjunct professor at the University of Notre Dame where he teaches pre-meds the art of “being with”.
Marcus lives in Orlando, FL with his wife Marvelyne, and his Seeing Eye dog, Elliott. He is, in his words, a social media junkie and loves to connect with healthcare professionals nationwide. All social media information can be found at www.marcusengel.com

Kevin Khoury received his Bachelor’s Degree in Psychology and Pre-Med from Oklahoma State University and his medical degree from the University of Santiago. Early in his career Kevin realized that marketing and business development were his greatest interests.
Using his knowledge of healthcare and his business acumen, Kevin has worked alongside organizations and corporations who have shown major growth in profitability in the marketplace.
Kevin has served on numerous Boards for nonprofits including his latest Board position with the Lupus Foundation. He was inducted into the State of Oklahoma Chamber of Commerce Hall of Fame for Marketing and Promotions and he has worked with the State of Oklahoma since 2002 developing Workers Compensation Symposiums.
Kevin enjoys volunteering and mentoring. He is an equestrian, vocalist, writer and guest speaker at schools, churches and civic organizations.
More information about Kevin can be found at khourycommunications.com.



Why We Exist
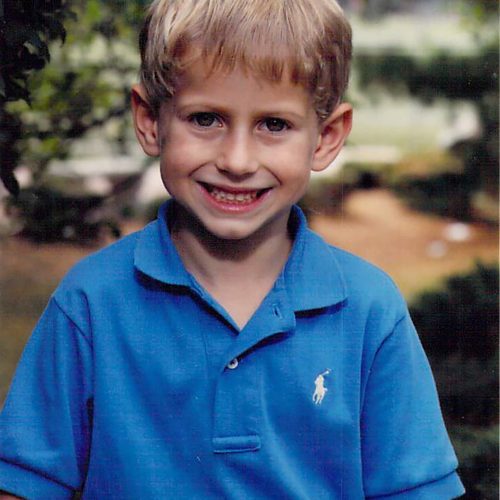
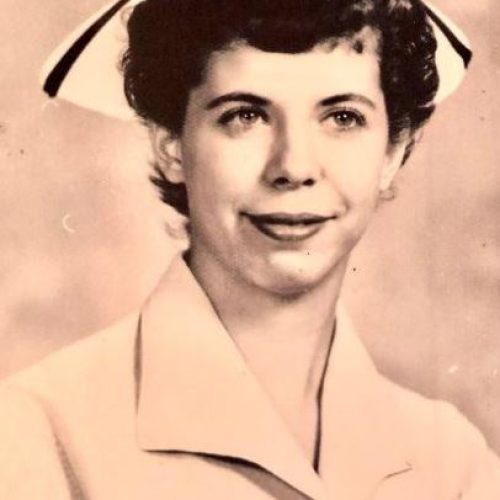
The Mom & Mitchell Foundation is named for founder Tim Jones’ mother and son, both of whom died by suicide. His maternal grandmother also died by suicide when his mother was a young girl.
Tim was only 11 years old when his mom was first hospitalized following a suicide attempt. Later in his teen years, he helped restrain his mom to prevent her from jumping from a second-story window. Despite many interventions through the years, including voluntary hospitalization, she ultimately took her own life at the age of 41.
Tim’s youngest son, Mitchell Brantley Jones, died by suicide at the age of 24. Mitchell had previously battled drug addiction and been in recovery, but he relapsed in 2017. On July 4 of that year, he ended his life.
In honor of his mom and son Mitchell, Tim started the Mom & Mitchell Foundation to raise awareness about the importance of mental wellness and bring hope to individuals and families who are struggling.
Why we need the Mom and Mitchell Foundation
The path to suicide for my grandmother, my mother, and my son were all different. Interestingly, I never, ever once remember my mother talking about her biological mother and her death. My mother had bipolar disease compounded by substance use. My son had severe anxiety. He compensated with alcohol and drugs and became addicted. Sadly, and ultimately, they all decide to quit on life.
The word ‘disease’ is an Anglo-French word, derived from 2 French words. ‘Des’ (dis), which means ‘not’, and ‘Eise’ (ease), which means ‘not stressed’, ‘relaxed’ or ‘comfortable’. Fundamentally, the word ‘disease’ includes anything that makes one uneasy. We classify diseases as mental or physical, but, in reality, they are intertwined and one influences the other. I have spent my entire professional career trying to help people relieve or manage human ‘dis-ease’. Practicing plastic surgery and ENT for over 35 years has taught me a lot about the health and mind of human beings. You learn what makes people well, or not. You see the consequences.
The Mom and Mitchell Foundation is needed now more than ever. Emotional stress and distress are at an all-time high as a result of the Covid-19 pandemic. The viral pandemic has created mental and physical disease. Morbidity and mortality in both mental health and physical health have increased. Everyone is more anxious. Many have turned to substance use, which, in turn, has led to the highest rate of overdose deaths ever. Federal and state policies intended to ‘treat’ the pandemic have been counterproductive and ill conceived. One could argue the government’s ‘management’ of the pandemic has created more mental and physical health problems. The Mom & Mitchell Foundation is being created to raise public awareness of mental health and wellness, educate the public on mental health issues, promote activities to improve health and wellness, and reduce the morbidity and mortality resulting from psychological and psychiatric diseases.
In the USA healthcare system, mental health wellness and treatment of mental disorders have not received the public attention and research funding that physical disease have received. Of the top Forbes 100 non-profit organizations in the USA, the far majority of organizations focus on a physical health problem like heart disease or cancer – (7) heart, (1) kidney disease, (1) Alzheimer’s, and (7) institutions/hospitals. There is only one non-profit organization in this list that focuses on mental health and wellness, the National Society for Mental Wellness.
Suicide is a major cause of death in the USA and worldwide. Each year over 30,000 people in the USA and approximately 1 million people worldwide die by suicide. Suicide represents our society’s failure in treating mental health disorders and diseases. Suicide has changed my life and my family’s lives and legacies. My maternal grandmother, my mom, and my only son, Mitchell, all decided to take their own lives. Suicide deaths are like pipe bombs – they kill the person who detonated the bomb, and the collateral damage maims all those around him/her. Relationships of surviving family and friends are inflamed and changed forever, many times never recovering.
Adolescence and early adulthood are the times of greatest risk for first onset of suicide behavior. It is the 2nd leading cause of death in youth ages 10-24. Data collected by the National Center for Health Statistics shows that suicide rates in youth aged 10-24 have increased by 57% between 2007 and 2018 from 7 in every 100,000 people to 11. Other groups with increased risk of suicide, include those with mental disorders, military personnel and veterans, and physicians.
There are known risk factors for suicide and suicide behavior. Demographic risk factors for suicide include male sex, being non-Hispanic White or Native American, and being an adolescent or older adult. The presence of a psychiatric disorder is among the most consistently reported risk factors for suicide behavior. Mood, impulse-control, alcohol/substance use, psychotic, and personality disorders convey the highest risks for suicide and suicide behavior, and the presence of multiple disorders is associated with especially elevated risk.
Most theoretical models of suicide behavior propose a diathesis-stress model in which the psychiatric, psychological, and biologic factors (serotonin metabolism) predispose a person to suicidal behavior, while stressful life events interact with such factors to increase risk. Consistent with such a model, suicidal behaviors often are preceded by stressful events, including family and romantic conflicts and the presence of legal/disciplinary problems. The experience of persistent stress also may explain why persons in some occupations, such as physicians, military personnel, and police officers, may have higher rates of suicidal behavior; however, this increased risk may be explained by the demographic and personality characteristics of people who select such occupations.
Prevention and treatment of physical diseases and disorders have always been the top priority in the USA healthcare system. And we have made great strides in eradicating and treating many potentially deadly physical diseases, including infectious diseases, heart disease, and many types of cancers. Quality of life and longevity from physical diseases have improved dramatically. But that cannot be said for mental health disease. There are many reasons for this discrepancy. Physical diseases are more prevalent. Heart disease and cancer are the #1 and #2 leading causes of death. Most physical diseases can be seen, imaged, or measured with a blood test. On the contrary, mental and psychiatric disorders are often hidden or masked, many times behind the physical disorder created by the mental imbalance, for example, substance abuse. Most importantly, there has always been a stigma associated with mental health disorders.
Prevention programs exist and can be effective in reducing suicide rates. Programs that restrict access to lethal means and training physicians to recognize and treat depression and suicidal behavior have shown impressive effects in reducing suicide rates. Although effective prevention programs exist, the fact that many people engaging in suicidal behavior do not receive treatment of any kind underscores the need for greater dissemination of information and further development of prevention efforts.
There are protective factors that decrease the probability of an outcome in the presence of elevated risk. Studies show those with religious beliefs, religious practice, and spirituality have been associated with a decreased probability of suicide attempts. Perceptions of social and family support and connectedness have also been studied outside the context of religious affiliation and have been shown to be significantly associated with lower rates of suicidal behavior.
When a person commits suicide, their family and friends become victims of suicide. It is a major psychological trauma that is lifelong. Helping the victim family members and friends transform from suicide victim to suicide survivor is one of the goals of the Mom and Mitchell Foundation.
The collateral psychological damage to surviving family and friends is profound. There is blame and finger pointing. Communications between family members ease for years, and sometimes forever. The psychological injury and hurt from losing the suicide victim are compounded by the destruction of family relationships that occurs afterwards. Failure to properly grieve and understand the loss can lead to lifelong psychological conflict.
My 2 brothers and sister also lost their mother. My 2 brothers together have 6 children. Nine grandchildren never knew their grandmother. My sister, 3 years younger than me, decided not to have children. She thought would pass down the gene the ‘suicide’ gene.
Following our mother’s death in 1973, our mom’s side of the family essentially vanished. For the next 40 years, we had no contact or communication with our 3 uncles/aunts and their children (6 cousins). Approximately 15 years ago, one of our female cousins who we had not met, Faith Catherine Warren, became interested in knowing the person she was named after. She reached out, re-establishing a family connection. This relationship has been personally beneficial, but the scars from the earlier years remain.
It takes time, spirituality, and insight to make transition from suicide victim to survivor. And, it is not always straightforward and linear. Some people never make the transition to survivor, and they continue struggling as a victim. My brother, David, took his experience as a survivor and made a positive difference. He became an elementary school counselor, helping high risk kids and families deal with suicide, addiction, abuse, and all that goes with it. He has had thousands of conversations that were only possible and credible because he was a “survivor”.
In many ways, this organization represents my quest for redemption. Redemption comes with helping others and helping others help themselves. After practicing medicine for almost 40 years, one observation stands out. People are more anxious. Living is causing more anxiety. Learning how to build mental resilience and develop more effective treatments for mental health disorders are needed now more than ever. Please join us in fostering mental wellness and happy minds.
